Macromastia is a medical condition that can lead to serious consequences for the spine and a patient’s mental well-being. Although breast reduction surgery is considered a medically necessary treatment in many cases, whether it is categorized as “cosmetic” or “reconstructive” determines the eligibility for insurance reimbursement. To understand exactly which cases qualify for financial assistance and find the answer to does insurance cover breast reduction, please refer to this article.
Does insurance cover breast reduction?
Whether or not your policy provides coverage depends heavily on whether the procedure is performed for medical necessity or cosmetic reasons. Generally, if you undergo surgery solely for aesthetic purposes to achieve a more balanced physique, insurance providers including both public health insurance and private health plans will decline to cover the costs.
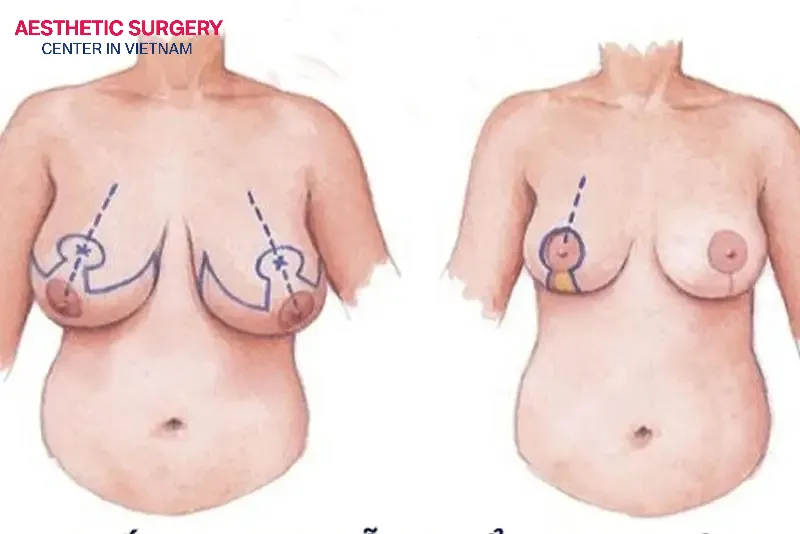
However, if you are diagnosed by a doctor with macromastia (breast hypertrophy) that causes serious health consequences—such as chronic back, neck, and shoulder pain, spinal deformity, or skin ulceration under the breast fold the surgery may be considered a medically necessary treatment.
To qualify for benefits, patients usually undergo a rigorous assessment process to prove that conservative treatments have been ineffective. Furthermore, the volume of breast tissue intended for removal must meet specific thresholds defined by each insurance provider. Therefore, before proceeding, you should carefully review the exclusion clauses in your policy and obtain a medical necessity certificate from an authorized hospital to maximize your chances of reimbursement.
Which types of insurance cover breast reduction surgery?
To determine which insurance will cover the procedure, it is essential to distinguish between the various nature of the surgery. Below are the details for each type:
Public health insurance (social health insurance)
Public Health Insurance generally does not cover elective cosmetic surgeries based on personal preference. However, if the oversized breast condition is diagnosed as a pathological hypertrophy causing severe health complications such as spinal pain, skeletal deformity, or chronic skin ulcers you may be eligible for benefits.
To receive coverage, the surgery must be performed at public hospitals (e.g., Military Central Hospital 108, Cho Ray Hospital, etc.) with a clear treatment indication from a specialist. In such cases, the coverage rate will follow regulations for correct-line or cross-line referrals (typically ranging from 40% to 80% of the approved medical list).
Private health insurance
Private health insurance policies typically have a very strict list of “exclusions” regarding plastic surgery. To qualify for coverage, a breast reduction surgery must be proven “medically necessary” rather than for cosmetic purposes. This requires you to provide comprehensive medical records proving that pathological symptoms were treated conservatively (e.g., through physical therapy) but remained ineffective. Some major insurance providers may also require a minimum volume of tissue removal to be considered for reimbursement under inpatient benefits.
Direct billing at international hospitals
If you use insurance cards with direct billing benefits at international hospitals (such as FV, Vinmec, or Tam Anh), the process is more convenient, but the requirements for medical evidence remain very stringent. In these cases, the hospital will work directly with the insurance company to confirm whether your breast reduction surgery falls within the scope of coverage based on your actual clinical examination results.
Typically, costs such as room fees, laboratory tests, and a portion of the surgical fees may be covered if the procedure is determined to be for correcting functional defects or pathological conditions.

What do insurance companies typically require to cover breast reduction surgery?
To obtain insurance approval for a breast reduction (reduction mammoplasty), you must prove that the procedure is medically necessary rather than cosmetic. Below are the specific requirements for the categories you are interested in:
Symptoms that demonstrate medical necessity
Insurance providers generally require clear evidence that excessively large breasts are causing chronic health issues. The most common symptoms include persistent neck, shoulder, or lower back pain that does not respond to standard rest or conservative treatments. Additionally, the presence of deep, painful shoulder grooving caused by bra straps is a significant indicator that the weight of the breast tissue is placing excessive pressure on the musculoskeletal system.

Dermatological and neurological complications
Beyond musculoskeletal issues, insurance companies also consider dermatological complications. Typical medical signs include chronic rashes, skin ulcerations, or recurrent infections in the inframammary fold (the crease under the breast) caused by moisture and friction.
Furthermore, if you experience numbness or weakness in your fingers due to nerve compression syndromes related to breast weight, these serve as “compelling evidence” to convince the insurance company of the surgical necessity.
Documentation of conservative treatment
Most insurance providers will not approve surgery immediately; instead, they require documentation proving that you have attempted non-surgical treatments for a specific period, typically 3 to 6 months. This documentation must include a log or medical records detailing your participation in physical therapy, strength training exercises for back and neck muscles, or the use of prescribed pain relief and anti-inflammatory medications that failed to provide long-term relief.
Additionally, conservative treatment records may include consultations regarding supportive garments, such as using specialized supportive bras designed to redistribute weight. If you experience skin issues, records from a dermatologist regarding the use of topical creams or antifungal powders for recurring infections should also be attached. A lack of documentation regarding these conservative treatment efforts is the most common reason for claim denials.
Estimated tissue volume and the schnur scale
One of the most critical quantitative criteria used by insurance companies is the volume of tissue expected to be removed during surgery. Typically, the surgeon must estimate the number of grams of breast tissue to be removed from each side. If this figure is too low—often under 500g, depending on the provider’s policy the insurance company may categorize the procedure as cosmetic plastic surgery rather than a medical necessity. The amount of tissue removed must be substantial enough to truly relieve pressure on the patient’s body.
How much does breast reduction surgery cost if covered by insurance?
Even if your breast reduction surgery is deemed “medically necessary,” the actual out-of-pocket amount you will pay depends on the type of insurance you hold and your specific policy’s benefit limits. Here are the estimated costs for common scenarios:
For public health insurance (social health insurance)
If you undergo the procedure at a public hospital with a valid medical referral (proper level of care):
- Coverage level: Public insurance typically covers 80% to 100% of the costs listed in the State-regulated price list (such as hospital beds, tests, and basic medical supplies).
- Out-of-pocket cost: You are usually responsible for the co-payment (20%) and any non-covered service fees (such as elective surgery fees, choosing a specific surgeon, or premium medical supplies). Total self-paid costs can range from 5 – 15 million VND.
>>> See more: How much does breast reduction cost?
For private health insurance
The amount covered depends entirely on the Inpatient Treatment limit in your contract:
- Full coverage: If the surgery cost ranges from 40 – 80 million VND at reputable private hospitals and remains under your maximum per-treatment limit, the insurance may cover 100%.
- Proportional coverage: Some plans specify a co-pay ratio (e.g., you pay 20%, insurance pays 80%). In this case, you might spend around 8 – 16 million VND.
Note: Private insurers tend to have strict exclusions for “cosmetic surgery fees.” Therefore, the actual approved amount may only focus on room charges and diagnostic tests.
We hope this article has helped answer your questions regarding does insurance cover breast reduction and the associated costs. In reality, the line between cosmetic surgery and medical treatment in these cases is quite thin. Therefore, obtaining confirmation from both your doctor and your insurance provider is the most crucial step you cannot skip. Follow us for the latest useful insights on insurance and medical aesthetics!



























Comment on the post